About Bowel Cancer
What is Bowel Cancer?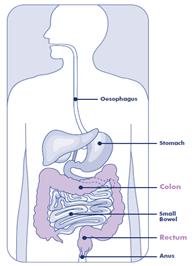
Bowel cancer occurs when the normal cells in the large bowel (also known as the colon) or rectum grow abnormally and form a lump or tumour. If not removed, the tumour can go on to spread throughout the body and eventually cause death.
What is a Bowel Polyp?
Most bowel cancers start as a non-cancerous growth, or polyp, in the lining of the colon. These polyps can take ten years or more to become cancerous. There are two common types of polyps:
- Hyperplastic polyps, which are the most common and do not appear to progress to bowel cancer.
- Adenomatous polyps (also known as adenomas), which are more dangerous. Some of them can progress to bowel cancer although they usually have to grow to about 1cm in size before any cancer develops.
About 30% to 40% of people over the age of 60 have one or more of these adenomatous polyps in the bowel but, fortunately, only about 5% of these will become cancerous. However, all adenomatous polyps should be removed so that the polyp tissue can be examined under the microscope to determine whether there are any pre-cancerous changes developing.
When you have a colonoscopy, to screen for bowel cancer, these pre-cancerous polyps can usually be removed at the same time.
Early detection and removal of polyps in a correctly designed screening and surveillance programme reduces the risk of dying from bowel cancer by approximately 60%.
Bowel Cancer – Are YOU at Risk?
- Approximately 70% of bowel cancer develops in people who have no known family history of bowel cancer.
- Having close relatives who have developed bowel cancer or precancerous bowel polyps increases your risk. The risk increases with the number of relatives affected.
- 1 in 18 New Zealanders develop bowel cancer.
- New Zealand has the highest rate of bowel cancer in the world.
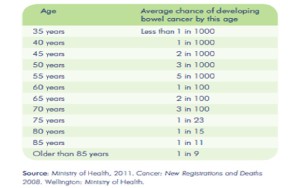
- 90% of bowel cancer occurs in people over the age of 50.
- Bowel cancer is the second most common killer in New Zealand (after lung cancer).
- Each year, about 2800 people in New Zealand develop bowel cancer and, each week, approximately 22 New Zealanders die of bowel cancer.
- Screening, surveillance, diet and exercise can significantly reduce the risk of dying from bowel cancer.
- Some diseases affecting the colon (such as ulcerative colitis or Crohn’s disease) are associated with a higher risk of colon cancer and this risk is higher if the condition has existed for eight years or more.
- Some uncommon genetic conditions (such as familial adenomatous polyposis and hereditary non-polyposis bowel cancer) also increase your risk.
- Having previously been affected by other cancers (such as cancer of the uterus, breast, ovary and small bowel) also increases the risk.
- Other factors that may increase your risk: smoking, a sedentary lifestyle, obesity, diabetes, heavy alcohol use, a diet high in animal fats and low in fruit and vegetables. Eating processed meats and more than 500g of red meat per week.
Are there any SIGNS of Bowel Cancer?
- There are usually no signs of early bowel cancer.
- Nor can you usually tell if there are any pre-cancerous polyps in the lining of your bowel. Without screening, bowel cancer can be a silent killer. Signs of it often arrive late when the cancer may be well advanced and more difficult to treat successfully.
- These late symptoms can include:
- rectal bleeding (which should never be ignored)
- weight loss
- anaemia or iron deficiency
- changes in bowel habit such as long periods of diarrhoea or constipation, a bloated stomach and wind or a sense of incomplete bowel motions
A referral to The Endoscopy Clinic for bowel cancer screening can give you peace of mind. Download Endoscopy Referral

